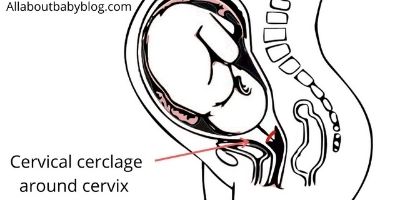
Prevent preterm birth with a cervical cerclage
A Cervical Cerclage can be a great way to keep your baby in the uterus longer.
Unfortunately some women experience difficulties during the third trimester including preterm labor and shortening of the cervix.
The cervix should not be getting shorter until it’s actually time to have the baby so when the cervix starts to get shorter and open up it can cause preterm birth way too early or a very late miscarriage.
Thankfully modern medicine came up with a great procedure called cervical cerclage to prevent that from happening.
The success rate it’s about 80 to 90% for a planned cerclage and 40 to 60% for emergency ones according to Wikipedia.
What is a cervical cerclage?
A cervical cerclage or cervical stitch is just that – stitches through the cervix.
It is performed in a hospital or surgical center with local anesthesia and most women can just go home after.
During the procedure the doctor will stitch around and through the cervix with a strong suture.
The word cerclage actually comes from the French language and literally means hoop – you see what they did there?
It can be done early in the pregnancy around 12 to 14 weeks and is removed later in the third trimester when the greatest risk of miscarriage is gone.
Cerclages that are performed after 14 weeks are usually emergency cerclages and you will most likely need another cerclage in future pregnancies according to WebMD.
It can be done up to 23-24 weeks of pregnancy if you don’t have any history of preterm birth or preterm labor.
While there is no guarantee for success the statistics speak for themselves.
Success rate 80-90% for planned cerclages and 40-60% for emergency procedures.
Source: Wikipedia
It is considered a success when it delays the delivery to at least 37 weeks when the baby is considered to be full-term.
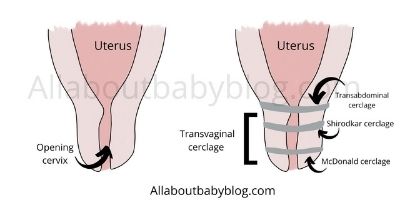
Types of cervical cerclage
There are two different types:
The McDonald cerclage
which is the most common – is basically a purse string stitch to close the cervix shut.
It is performed on the upper part of the cervix.
This type can be done around 16-18 weeks of pregnancy.
The Shirodkar cerclage
Is very similar to the McDonald method but goes through the cervix walls and the suture is not exposed.
Both are being removed around 37 weeks of pregnancy.
Cerclages can be performed transabdominal with a little incision through the stomach which is less common and requires a full surgery or transvaginal.
The transabdominal cerclage is only done when it is not possible transvaginal.
If you do end up having a transabdominal cerclage your doctor will most likely reccomend you having a C-section around 37 to 39 weeks of pregnancy.
Women can experience light cramps and spotting for a few days after the procedure is done.
Why do doctors perform cervical cerclage?
Before and at the beginning or your pregnancy your cervix is long and firm.
During the course of pregnancy it slowly starts to become softer, effaced (becomes shorter) and opens up the closer you get to delivery.
If the cervix becomes too short too soon it can start to open and send you into preterm labor.
To prevent that your doctor may advise you to have this procedure done especially in the following cases:
- a history of late pregnancy loss or late miscarriage
- Painless dilation in the second trimester
- Active preterm labor
Source: mayoclinic
This may also be interesting:
– Signs of labor
– Paid maternity leave in California
– Membrane sweep – the easy labor starter?
– Early pregnancy symptoms
Does it hurt?
During the surgery you will anesthesia to prevent pain and most likely experience some discomfort after.
Your doctor may prescribe you some light medication.
What are the risks?
The risks of a cervical cerclage can include:
- vaginal bleeding
- Inflammation because of bacterial infection
- Tearing of the cervix
- Premature water breaking
- Displacement of the surgical suture
You should contact your doctor if you experience any of these symptoms.
Especially when you experience that there is any fluid leaking from your vagina – if the amniotic sac breaks early the cerclage might have to be removed.
However some light spotting and cramping is normal for some days after.
However if you do feel like it is more spotting or bleeding and cramping than there should be don’t hesitate to contact your doctor right away just to make sure everything is ok.
Complications from a procedure like that are very uncommon and less than 10% of all cases when you have a planned cervical cerclage.

How to prepare yourself
You will have an appointment with your doctor for an ultrasound to check your baby’s vitals and make sure there aren’t any birth defects.
Your doctor might also take a swab around your cervix to check for any infections.
Sometimes the amniotic fluid is checked too with a needle through your stomach into the uterus.
If you do have any infections you might need to take antibiotics and wait until the treatment is done.
This may also be interesting:
– 10 Pregnancy announcement ideas
– Funny pregnancy stories
– 10 creative gender reveal ideas
– Epidural vs. natural birth
When should it NOT be done?
sometimes even when your cervix starts to get shorter your doctor might not perform a cerclage when:
- you have a infection
- The baby has major anomalies that makes it unlikely to live
- Your water breaks before 37 weeks of pregnancy
- the amniotic sac squeezes through the cervix opening (called Prolapsed fetal membrane)
- You are pregnant with twins or more babies
Are there alternatives?
There is a silicone product called Arabin Pessary which is supposed to do the same job as a cerclage but without stitches or surgery.
Studies on this product however did not prevent premature birth as much as a classic cervical cerclage does.
That’s why the society of maternal-fetal medicine advises to only use the pressary as part of a clinical trial or research.
How much does a cerclage cost?
The average cost of the procedure alone for a simple transvaginal cerclage without an overnight stay is about $546 – $1,174 according to PubMed.
You can also always ask your health insurance about out of pocket cost for procedures before they are done.
What you shouldn’t do after a cerclage
Your doctor will tell you not to have sex or use any tampons or douches up to 24 hours after the procedure.
In general just take it slow and rest.
Did you have a cervical cerclage done?
Are you expecting a baby? Subscribe to my email list to get pregnancy and baby-related information, fun stories and the best offers for new moms. Plus a free printable Baby shower Bingo in your email.









